Each year, according to the Cleveland Clinic, an estimated 14 million people in the U.S. become infected by one of the dozens of variants of human papilloma virus, or HPV.
In many cases, infection by HPV—the most common sexually transmitted infection—causes no symptoms and is cleared from the body naturally by the immune system. However, sometimes infections can persist and, in addition to symptoms such as warts, eventually lead to cancer.
Most commonly associated with cervical cancer, HPV infection has been linked to other genital cancers as well as cancers of the head and neck, in both men and women. Worldwide, roughly 600,000 people are diagnosed with HPV-associated cancers each year. Thus, one of the most important public health challenges of the 21st century will be to minimize the impact of HPV infection and its related cancers.
Fortunately, with immunotherapy, there is hope.
Therefore, on this International HPV Awareness Day, we want to highlight how immunotherapy can—and already has—helped us against this pervasive and potentially deadly virus, thanks in part to the work of Cancer Research Institute (CRI) scientists.
Preventing HPV Infection
Since HPV appears foreign to the immune system, vaccines can be used to teach the immune system what HPV looks like, molecularly speaking. Then, the immune system can recognize it and eliminate it along with any cells that become infected.
In 1999, CRI started funding the work of Ian H. Frazer, MD, AC, FRS, FAA, of the University of Queensland in Australia, who helped develop Gardasil, the first vaccine designed to prevent HPV infection. To do so, Dr. Frazer and his colleagues developed a technology for producing synthetic HPV-like particles, and then tested this approach in clinical trials with CRI’s support.

Dr. Ian Frazer
“It’s the genetic material inside the virus that causes all the trouble,” said Frazer. “We realized that if we could manufacture the harmless outside shell of the virus we would have the basis for a vaccine to prevent cervical cancer.”
In 2006, Frazer personally administered the first dose of Gardasil, which protects against four variants of HPV, and the FDA soon approved it for use in young women. That same year, he—along with Harald zur Hausen, MD, who first discovered the role of HPV in cervical cancer—received the William B. Coley Award for Distinguished Research in Tumor Immunology, CRI’s highest scientific honor.
Since then, two additional preventive HPV vaccines have been approved by the FDA, which have collectively been used to immunize hundreds of millions of people globally.
Ideally, these vaccines are given to people before they are exposed to HPV, in order to prevent the virus from infecting them in the first place. However, as Frazer has noted, "Half-a-million women already exposed to HPV will continue to develop cervical cancer every year, and half of those women will die.”
As a result, new HPV-targeting immunotherapies are urgently needed for the many people who have already been infected by the virus or developed HPV-associated cancers.
“A therapeutic cervical vaccine,” said Frazer, “will take a lot of work to go from the lab to a real product. But as long as funding continues, I’d say we could well have a therapeutic vaccine for cervical cancer within the next decade.”
Treating HPV-Associated Cancers
Fortunately, the funding has continued, and the work of another CRI scientist—Cornelis J. M. ‘Kees’ Melief, MD, PhD, of the Leiden University Medical Center—has advanced this promising approach to the clinic.

Dr. Cornelis Melief
Dr. Melief, who would go on to receive the 2009 William B. Coley Award as well as the 2019 AACR-CRI Lloyd J. Old Award in Cancer Immunology, first set his sights on helping people infected by HPV who have a form of pre-cancerous disease known as high-grade vulvar intraepithelial neoplasia, or VIN3. In one clinical trial, Melief’s HPV-targeting vaccine led to responses in roughly half of the patients treated, and many experienced long-lasting benefits.
By itself, however, this vaccine wasn’t effective for patients who had already developed advanced, HPV-positive cervical cancer. More recently, in an effort to help these patients, Melief and his colleagues have explored combination strategies to enhance the effectiveness of HPV-targeting vaccines.
Thus far, they’ve found that combining HPV vaccination with chemotherapy can provide great clinical benefit in patients with advanced cervical cancer. Additionally, in patients with incurable, HPV-positive head and neck cancer, combining HPV vaccination with checkpoint immunotherapy doubled the response rate and median overall survival of patients compared to checkpoint immunotherapy alone.
For some people with advanced, HPV-positive cancer, checkpoint immunotherapy alone can be enough. Poison drummer Rikki Rockett’s metastatic oral cancer was completely eliminated after he was treated with pembrolizumab (Keytruda®), a PD-1 checkpoint inhibitor, in a clinical trial.
Dr. Melief and others continue to explore these and other novel strategies, including a triple combination of HPV vaccination, chemotherapy, and checkpoint immunotherapy.
A Future Immune to HPV
HPV is responsible for approximately 90 percent of anal and cervical cancers; 70 percent of vaginal and vulvar cancers; 60 percent of penile cancers; and 60-70 percent of oropharynx cancers.
Thanks to the efforts of Dr. Frazer, Melief, and many others, it’s not inconceivable that we could eventually eradicate HPV infection altogether as well as the many cancers caused by the virus.
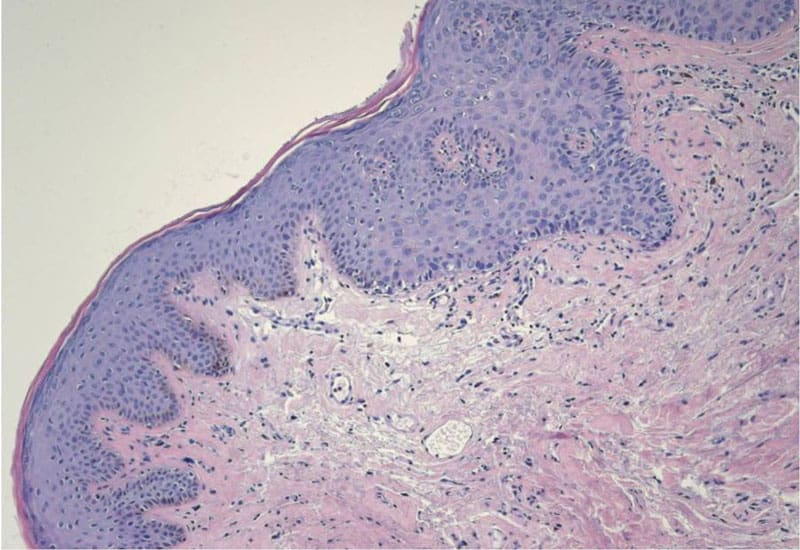
VIN lesion post-vaccination. Image courtesy of Dr. Cornelis Melief.
Achieving that goal will require significant and sustained efforts. In addition to improving the scope and scale of our preventive HPV vaccine practices, we must learn more about the basic biology behind HPV infection and HPV-related cancers, and how they interact with the immune system. A better understanding of the mechanisms at play might then enable us to develop even more effective immunotherapy strategies, including vaccines, that cover a wider range of HPV variants.
The remarkable progress we’ve made thus far against HPV and HPV-related diseases, combined with the considerable continued commitment to overcoming them, should give us all hope that we may one day be able to bring about a future immune to HPV.